

Do You Need Vitamin C on the Carnivore Diet?


High vitamin C supplementation has been touted as a miracle antioxidant for a variety of health benefits ranging from the ability to lower the risk of cancer to preventing cardiovascular disease. While vitamin C does play important roles across many physiological functions, one of the most common concerns about the carnivore diet is in regard to vitamin C and potential scurvy issues. However, this concern is generally rooted in the mainstream dietary fallacy that plants are the only source of vitamin C. There are also other nuances that impact your vitamin C requirements when eating an all-meat diet. Let’s take a closer look at vitamin C requirements and why this shouldn’t be a concern for those interested in starting or staying on the carnivore diet.
Vitamin C Requirements In the Body


Vitamin C is a water-soluble nutrient that’s naturally occurring in certain foods. This essential dietary nutrient isn’t produced by the body on its own. It acts as an antioxidant, helping protect cells from free radicals. Vitamin C is required in the body in order to:
- Promote collagen production
- Improve absorption of iron
- Support the immune system
- Metabolism of protein and cholesterol
- Proper wound healing
- Fight against oxidative stress
- Help produce neurotransmitters that impact mood
Carnivore Diet Background
Before we dive into the nuances of vitamin C on a carnivore diet, let’s discuss what the carnivore diet is and some of the important benefits it can offer.

The carnivore diet focuses solely on animal proteins and fats, eliminating all foods from the plant kingdom. It acts as the ultimate elimination diet and is a true zero-carb or nearly zero-carb way of eating. While there are many variations with the diet and even more reasons as to why individuals may decide to try carnivore, here are some of the main benefits available with this approach:
- Minimize plant anti-nutrients: Plant anti-nutrients including oxalates, phytic acid, and lectins can pose a number of issues when consumed regularly. This is especially true for individuals with any metabolic dysfunction or existing chronic illness. Anti-nutrients are found in various levels across all plant food categories such as vegetables, fruits, grains, beans, nuts, and legumes.
- Avoid mycotoxins and aflatoxins: Particular mold strains can produce mycotoxins which are toxic mold particles. Aflatoxins are a type of mycotoxin that is a known poisonous carcinogen. These mycotoxins are generally found in grains, nuts, coffee beans, spices, dried fruits, seeds, legumes, and more. A carnivore diet offers the opportunity to minimize ingesting these biotoxins and can be further reduced by opting for grass-finished meats only.
- Reduce glyphosate and pesticide exposure: Glyphosate is a dangerous herbicide that’s been established as a significant contributor to cancer. Pesticide exposure has been linked by countless studies to chronic illness, autoimmunity, and other short-term and long-term health effects. Eating a meat-only diet helps reduce ingested glyphosate exposure from genetically-modified crops, non-organic conventionally raised plants and grains, as well as many processed foods.
- Reverse chronic illness from excess sugar: There are a number of studies that support the increased risks of chronic illness with consuming excess sugar and carbohydrates. Overconsumption of these two compounds has a direct correlation with conditions including type 2 diabetes, cardiovascular disease, depression, and tooth decay. High consumption of fructose or glucose can also increase the body’s requirements for certain vitamins and minerals.
- Prevent fiber intake: Contrary to popular belief, high fiber intake can contribute to IBS, constipation, and other digestive issues. Studies show that a zero-fiber diet can reverse digestive symptoms including bloating, IBS, and constipation. Fiber isn’t ideal for individuals with SIBO and can add additional roughage that’s difficult for any compromised digestive system to process.
- Avoid processed and inflammatory foods: Processed foods and inflammatory vegetable oils are significant drivers of modern chronic illnesses. While foods in both categories can be considered plant-based, they pose serious health risks and concerns. A carnivore diet eliminates all processed and inflammatory foods, providing the cleanest, most anti-inflammatory diet possible.
- Most bioavailable, nutrient-dense diet: Meat offers the most bioavailable nutrients. If only eating plant-based, individuals will experience nutritional deficiencies without proper supplementation. Vitamins B12, D3, EPA, DHA, taurine, and creatine are not found in plant foods. Vitamins A, E, iron, and zinc are also very low in plant foods. All of these nutrients are essential for optimal wellness and physiological function. Animal protein and amino acids are also far superior when compared to plant sources in terms of quality and bioavailability.
From gut healing to autoimmunity remission, the carnivore diet is a powerful intervention for promoting root-cause healing or supporting individuals on their root-cause healing journey. Based on our clinical practice and mounting scientific data, there are so many benefits and reasons to try this dietary approach.
Vitamin C on the Carnivore Diet?
So, should we be concerned about getting enough vitamin C on a carnivore diet? Let’s take a deeper look at these potential issues and debunk common dietary and health myths that this concern is rooted in.
Scurvy
Scurvy is characterized by severe vitamin C deficiency. Since vitamin C plays so many various roles throughout the body, a deficiency can lead to widespread symptoms. Scurvy generally begins after at least four weeks of severe, continual vitamin C deficiency but requires at least three months for symptoms to occur. In the US, 7.1% of people may develop a vitamin C deficiency but extreme deficiency such as scurvy is very rare. Early symptoms of deficiency include weakness, fatigue, and sore arms and legs. Without treatment, decreased red blood cells, gum disease, changes to hair, and skin bleeding may occur.
Carnivores have pretty much debunked the worries over scurvy. Of the hundreds of meat-based clients we’ve worked with where the carnivore diet wasn’t fully working, not one client was unwell because of a vitamin C deficiency. Major drivers as to why these clients weren’t doing well include not enough fish or fatty acids, too much liver consumption, not enough fat intake, not enough meat intake, as well as other root causes such as CIRS. But never has vitamin C deficiency been the culprit.
Vitamin C In Meat


According to the USDA, muscle meat contains no vitamin C. However, this is factually inaccurate and based on the default practice of the USDA to fill in vitamin C amounts as “assumed to be zero”. This is a serious error considering that the USDA tests for almost all other micronutrients. Luckily, there are studies proving that there are naturally occurring vitamin C levels found in meat. If you ever experience any of the symptoms of vitamin C deficiency as listed above, you can always eat some of the meats with vitamin C. These symptoms can also be due to mineral or electrolyte imbalances as well as thyroid imbalances.
The recommended daily allowance (RDA) of vitamin C was created based on the minimum intake required to maintain near-maximal neutrophil concentration for antioxidant protection, not to prevent vitamin C deficiency. In order to avoid scurvy, you only need 10mg of vitamin C per day. The RDA for vitamin C for adults 19+ years old is 90mg for males and 75mg for females. Pregnancy RDA is 85mg and lactation RDA is 120mg. It’s recommended that smokers ingest an additional 35mg daily.
Pork liver (25.3mg per 100g serving) and chicken liver (17.9mg per 100g serving) do have measurable amounts of vitamin C while beef liver only has about 1.3mg per 100g serving. However, always limit the amount of liver you’re ingesting in case of hypervitaminosis, excess copper, and high purine levels. Many of these animal food sources consumed in 200g servings (7 ounces) will cover your RDA of vitamin C, including eating muscle meat alone.
Low-Carb Diets
When eating a low-carb diet, your need for vitamin C is reduced. That’s because glucose and vitamin C use the same receptors. So without glucose in the body, the same receptors for vitamin C won’t have to fight off glucose from the bloodstream in order to nourish the rest of the body. For example, oranges are rich in vitamin C– for every 100g, it has about 130mg of vitamin C but also has 25g of carbs. Perhaps oranges are designed to have more vitamin C because it has to compete with glucose for uptake. Those eating a high-carb diet will likely require a higher amount of vitamin C, but this differs for those eating a low-carb or carnivore diet.
Consumption of refined sugar reduces white blood cell function. White blood cells make up the immune system with 70% to 80% residing in the gut. Studies show that a high-sugar diet abnormally impacts the innate immune system, which includes increased inflammation. Our adrenals produce hormones like cortisol to manage insulin and blood sugar levels. Lowering sugar consumption will require less cortisol production. If the body is stressed and sleep-deprived, cortisol will continue to release. A high-sugar diet and a stressful lifestyle overtax the adrenals that make cortisol. One nutrient that supports hyperfunctioning adrenals is vitamin C. What if vitamin C needs have increased because of the confounding factors of a high-sugar diet, a stressful and sleep-deprived lifestyle, and overall adrenal imbalances?
Questionable RDA Values
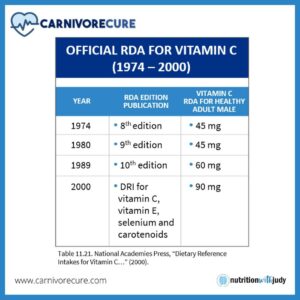


In 1974, the RDA for vitamin C in men was 45mg. The RDA increased to 60mg in 1989 and again to 90mg in 2000. Sure, science is a thing. But, did we really progress and learn that we need double the amount of vitamin C in just 26 years? It’s been 21 years, are we due for another uptick? Or is this progressively increasing RDA a direct correlation between the heightened need for vitamin C for those eating high carbohydrates and sugar found in the Standard American Diet?
Corn subsidies made high fructose corn syrup (HFCS) rise to notoriety, leading to a shift in all sodas in 1984 as sugar was swapped for HFCS. During the mid-1990s, GMO corn started appearing, creating a significant difference in processed foods and the way we eat. The timing eerily lines up with the increase in vitamin C requirements. Which poses the question– is an increase in vitamin C a bandaid for the overconsumption of glucose-friendly carbs? What if we stop all the excess sugar and carbohydrates? Individuals on a low-carb or carnivore diet can anecdotally vouch for less vitamin C needed.
Gold Standard Breast Milk
We design our amino acid requirements for proteins around the makeup of breast milk. The daily RDA for vitamin C for zero to six-month-old babies is 40mg. This increases to 50mg for babies between seven and twelve months old. Breast milk will maybe have half that amount. Should we stop exclusively breastfeeding because it’s not making the vitamin C RDA cut? We have yet to hear about any babies with scurvy or vitamin C deficiency.
Is High Vitamin C Safe?
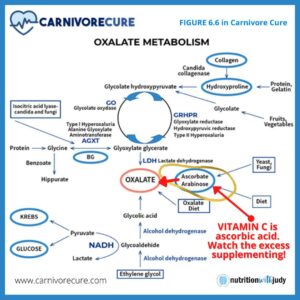

Anything in excess isn’t good. High vitamin C consumption can increase urinary oxalate acids and the excretion of uric acid, causing kidney stones. One of the metabolites of vitamin C is oxalic acid. If the body chooses to have ascorbic acid go down the oxalic pathway, you’ll have more oxalates. As vitamin C supports the absorption of nonheme iron in plants, excess iron absorption can also occur. The excess iron absorption can cause tissue damage.
While vitamin C is known for its antioxidant benefits, it can also act as a prooxidant in excess amounts, causing more oxidative damage. More oxidation means more inflammation in the body. Vitamin C supplements can cause DNA damage and may even contribute to cancer. Other studies have shown that high vitamin C consumption can reduce vitamin B12 and copper, cause quicker excretion of vitamin C, and produce allergic reactions.
Closing Thoughts for Vitamin C on the Carnivore Diet


While there can be a case made for certain individuals needing additional vitamin C intake, many don’t seem to need it. Eating fish, seafood, or organs (e.g., beef spleen, pork liver) can increase your vitamin C without having to eat things from the plant kingdom or risk additional supplementation. In our clinical practice, vitamin C hasn’t been an issue for any of our carnivore clients. We believe that all the different meats that have naturally occurring vitamin C simply show that eating a variety of meat on a carnivore diet is ideal. It might not be required but it is ideal for nutrient density.
Work With Our Trusted Carnivore Diet Functional Nutritional Therapy Practitioners
The Nutrition with Judy practice is honored to be a trusted carnivore diet practitioner support serving clients from around the globe. We’re passionate about helping our clients achieve root-cause healing in order to lead the best quality of life possible that’s nearly symptom-free. Our team is dedicated to educating our community about the incredible benefits of the carnivore diet. We welcome you to explore our free resources and are always available to support you through personalized protocols. Our Symptom Burden Assessment (SBA) is the perfect starting point for discovering your root cause and is required to work with our team— you can learn more in-depth about this powerful tool here.
Start your root-cause healing journey today and contact us any time with any questions or concerns.
DISCLAIMER: This content is for educational purposes only. While we are board-certified in holistic nutrition and are nutritional therapy practitioners, we are not providing medical advice. Whenever you start a new diet or protocol, always consult with your trusted practitioner first.





Craig A. Olson
October 13, 2023 at 4:20 amWhy would I want reduced weight loss?