
Written Interview with Chris Masterjohn, Ph.D.: Vitamin A and Consuming Liver


I never did a written interview before so this is quite exciting!
After the many vitamin A and liver interviews, posts and content, I reached out to a few of the pro-liver consuming advocates to get their thoughts on hypervitaminosis A. I don’t like naming names but they have verbally declined.
I told one doctor that when she is ready, the door is always open.
Many of you said to get in touch with Chris Masterjohn since he’s an expert with all things vitamins and minerals. He has kindly responded to a written interview.

My intent has always been to provide evidence-based research to best support the community. So unedited, here is the full interview:
Can you get vitamin A toxicity from just foods?
CM: While there is some controversy in interpreting specific examples of vitamin A toxicity from natural foods, there is no reason to believe that this toxicity isn’t just as possible. Natural foods do have factors that help balance vitamin A that would not be found when taking isolated vitamin A supplements, but the vitamin A would not be balanced by those factors sufficiently at all, if, say, you ate two pounds of liver per day. So it is better to stay on the safe side and limit liver to more traditional usage, such as once a week.
Specifically, on a meat-based carnivore diet? Say that a person eats 2 ounces of beef liver daily, 6 eggs, 4 tbsps of butter or ghee, and salmon too. And muscle meats that are more negligible?
CM: There’s no particular reason a carnivore diet would make one more or less vulnerable to vitamin A toxicity.
Vitamin A toxicity is very unlikely from this diet since it includes sources of vitamin D and the liver is kept to 14 ounces per week. However, I would recommend the average person limit liver to 8 ounces per week if they do not have any signs of needing more vitamin A.
How much would you recommend kids eat, for liver daily or weekly, that is safe? Say for a one-year-old? One ounce of liver or cod liver oil surpasses the daily UI (upper intake) limit. Is that a concern?
CM: It would be wise to limit the vitamin A from liver and cod liver oil to the tolerable upper intake level set by the Institute of Medicine. There is no guarantee of problems from those amounts, but there are some reports of infants and young children who have developed vitamin A toxicity symptoms from amounts that are exceeded by those foods, so there is no particular reason to use amounts that high unless the child has signs of vitamin A deficiency.


Some people say balancing various fat-soluble vitamins will help to offset vitamin A but the liver doesn’t have much vitamins D, E, K. Is this a concern?
CM: Yes. It is true that they offset each other’s toxicity, and the need for vitamin D, in particular, rises a lot when vitamin A intakes go up, because the two vitamins perform many functions together. Liver does not contain all the nutrients needed to balance the vitamin A by itself.
Do you think it’s possible that carnivores, eating lots of eggs, liver and dairy are risking toxicity with vitamin A? Or is the diet clean that it’s a non-concern?
CM: The concern would mainly come from the liver. If liver is limited to eight ounces per week there isn’t much of a concern.
If a person has a history of liver disease, is vitamin A toxicity a non-issue from foods?
CM: Someone with a history of liver disease is going to be much more vulnerable to vitamin A toxicity at lower doses.
What about if they used Accutane? (I’m trying to understand at what point is vitamin A something to caution for. Where I’m really struggling is why are there upper limits if some people ignore them?)
CM: Accutane has anti-vitamin A actions. Accutane can cause vitamin A deficiency symptoms that are relieved by vitamin A supplementation. I would not factor Accutane into the upper limit for vitamin A by assuming they add together.
Would you recommend anyone consume cod liver oil with levels of vitamin A?
CM: Cod liver oil can be a very useful source of vitamins A and D and long-chain omega-3 fatty acids. Whether someone should use it depends on the rest of their diet and whether it is adequate for these nutrients.
You said, “The majority of Vitamin A toxicity cases involve months or years of consistently taking more than 4620 IU per kg/day… however, vitamin A preparations that are water-soluble, emulsified, or solid may cause toxicity in weeks rather than months and at ten times lower doses.” Can you clarify?
CM: These are specific supplements designed for people with fat malabsorption. It does not include food, and if you are using a vitamin A supplement that does not say it is prepared in this way, it isn’t. Foods and almost any vitamin A supplement that doesn’t say it is emulsified require a higher dose for toxicity.
Chris Masterjohn has a vitamin and mineral cheat sheet if you are interested in more details on specific essential nutrients. You can find it here.
My Thoughts
It’s clear that you can get toxicity from vitamin A, even from food alone. And while Chris Masterjohn thinks 8 ounces of liver consumption is safe a week, some variables will change that amount. Your age, history with liver disease, fat-consumption load, even Accutane use (watch the interview with Dr. Garrett Smith for the studies). If you are also consuming other vitamin A-rich foods, the risk becomes higher.
From a pure mathematical view, if vitamin A content of 8 ounces of beef liver is safe a week, then once you add in egg yolks, butter, dairy, and other foods rich in vitamin A (there are many), the 8 ounces will inevitably lessen.




So How Much Is Right for You?
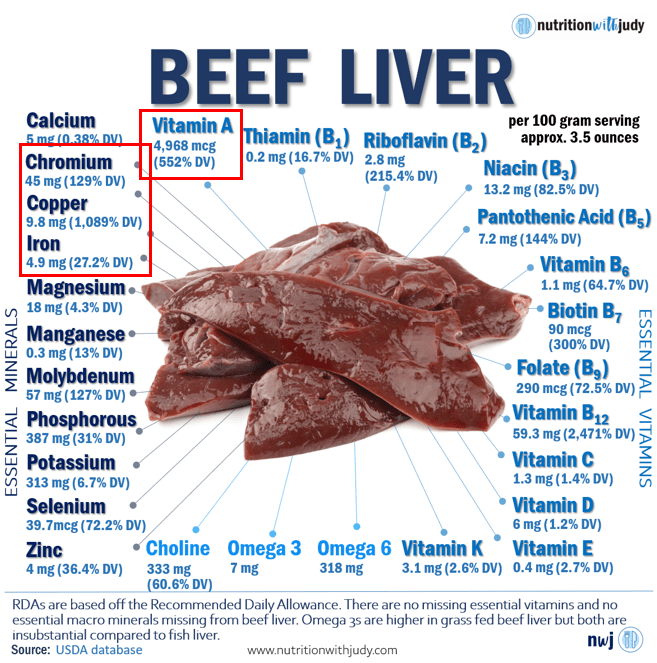
With animal liver containing large amounts of vitamin A (without much of any vitamin D), copper, chromium, iron, and B12 excess, I just wouldn’t risk it. You can read my breakdown on this here.
Anecdotal Client Share
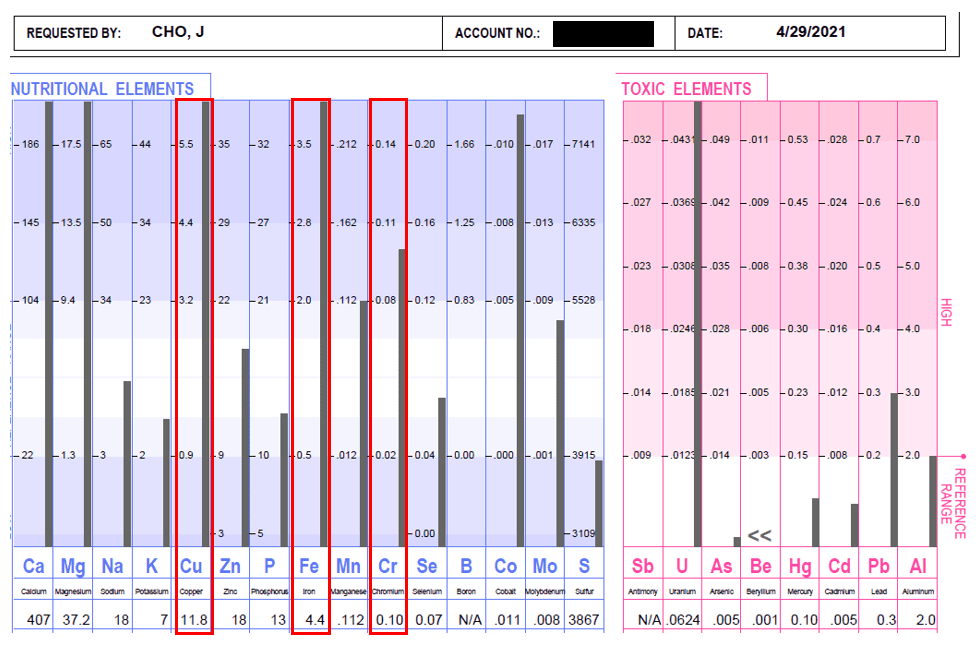
This client took a hair mineral test because he wasn’t feeling well. I can see why. He’s losing a lot of calcium from all the imbalances and if he’s taking D3, this is going to get worse.
He shows all the signs of someone consuming way too much liver. (He does). He has high iron, copper, and chromium. All things that liver is in excess. The minerals work antagonistically and synergistically together. We like to see a zinc: copper ratio of 8:1. My client is more copper than zinc. We need zinc to produce hydrochloric acid (stomach acid) to break down our meats in the stomach and then absorb nutrients later down in the small intestine.
He also has higher levels of heavy metals. Sometimes our body uses heavy metals to balance some of the nutritional elements that are inadequate so things within the body will still function. Remember, minerals are the spark plugs in our body and they make things happen. When there’s a deficiency, our body uses the best option it has.



So when people ask me if they should eat animal liver, unless they are severely nutrient-deficient, I would play it safe and advise against consuming liver. You can get every single essential nutrient with beef, eggs, butter, and salmon. You can read my blog post where I explain the nutrient density in a rainbow of carnivore meats.
In fact, if you want to eat liver, it’s wise to eat salmon with its high dose of vitamin D. We hear to stay away from mercury-filled, PUFA-rich salmon, but with the levels of Thiamin (B1) that are non-existent in beef and the better balances of the fat-soluble vitamins, it’s frankly a mistake.
Now if you can’t tolerate salmon because of histamines, then that is different.


Sharing my concerns about hypervitaminosis A was never about fear-mongering. I honestly have better things to do with my time. I hope the more light is shed on this discussion, you will realize that there’s a lot we are still learning with nutrition.
Science always evolves, even Recommended Daily Allowances have changed over the years.
Be open. Learn. Absorb. Then decide what makes sense for you with the new information. If we don’t stay open, we would never have learned the powers of a meat-based diet.
w️ith ♥ and hope for healing,


If you enjoyed this blog post, you may also enjoy these Nutrition with Judy blog posts:
- Liver and Risks of Vitamin A
- Don’t Eat Just Beef on a Meat-Based Diet
- Mineral Balancing and Sole Water
- Make Meat a Priority for You and Your Children
- What’s in Canola Oil
- Meat and Climate Change
DISCLAIMER: The content is for educational purposes only. While I am a nutritional therapy practitioner, I am not providing medical advice. Whenever you start a new diet or protocol, always first consult with your trusted practitioner.




Jane
June 19, 2021 at 4:03 pmThanks for that, Judy – very interesting.
I have the MTHFR gene mutation and have been taking beef liver capsules once a day, given that liver is supposed to be the best source of folate. I don’t consume liver in any other form, and my diet consists of about 3 eggs a day with some butter for one meal, and mostly either beef, fish or chicken for the other.
Do you think it is still best to steer away from liver for people with this gene mutation?